#2: Rotator cuff related pain.
Case series discussion #2: Rotator cuff related pain
Mrs R is a 63-year-old lady who was referred to Physio and Fitness Clinic by her GP, who suspected frozen shoulder after Mrs R reported experiencing increasing right sided shoulder pain and ‘stiffness’ for a period of three months. She had not experienced a traumatic event, although she recalled spending the weekend prior to symptom onset moving house which required lifting many boxes repetitively. By the time of presentation, Mrs R could not lift her arm above shoulder height due to pain and was unable to tolerate daily tasks including washing laundry and carrying household items that weighted more than one kilogram (e.g. lifting the milk out of the fridge). She also reported being unable to maintain her garden, which was particularly frustrating for her.
Mrs R reported pain to be primarily at the front of her shoulder, and while it was most severe with movement and under load (lifting activities), it was also painful at night when trying to sleep. She denied nerve-type pain radiating down her arm or other sensory disturbances, or neck pain. Objective testing revealed a greatly reduced and pain limited active range of motion through all shoulder planes; however, passive range of motion was only mildly reduced where pain limited motion. For example, Mrs R could only actively achieve 60 degrees of shoulder flexion due to pain, while passively this was 140 degrees before pain limited further range. On palpation, the biceps (long head) tendon was sensitised through the bicipital groove of the humerus. Additionally, the supraspinatus, infraspinatus and teres minor muscles were also sensitised, as was the posterior glenohumeral capsule.
Gravity resisted body weight external rotation (in left side-lying) through pain tolerable active range of motion resulted in short-lasting minor improvements to shoulder flexion and abduction active range of motion pain. The neck was investigated to rule-out radiculopathic pain, and active range of motion was regular and pain free. Based on subjective and objective findings, a diagnosis of rotator cuff related pain was made.
Initial physiotherapy intervention consisted of education for activity modification based on pain-guided criteria. If any activity provoked pain greater than 3/10 (where 0 = no pain, and 10 = worst pain imaginable) while being completed was discouraged. Likewise, if an activity resulted in increased/aggravated symptoms following completion and into the next day, it too was discouraged. Exercise was prescribed, starting with gravity assisted body weight active range of motion guided by the same pain criteria. This included ‘elephant trunk’ shoulder flexion and abduction. Isometric shoulder external rotation was also provided with a light theraband. Finally, pain modulation targeted therapy was applied in the form of soft tissue massage to the posterior glenohumeral joint capsule, and the supraspinatus, infraspinatus and teres minor over the scapula. To enable this pain modulation therapy to be replicated at home, self-applied massage ball therapy to this region was practiced with Mrs R.
After a week, Mrs R demonstrated improvements to pain tolerated active range of motion, although this was still greatly reduced compared to passive range of motion. Side lying external rotation was trialled with a 1kg dumbbell (figure one), which Mrs R found tolerable (<3/10 pain). This was prescribed in place of the theraband isometric exercise. Early range shoulder abduction was also trialled, tolerated and prescribed with a 2kg dumbbell, with the magnitude of range guided by pain tolerability. Mrs R was provided education on how to self-progress the side lying external rotation and early range shoulder abduction based on the pain tolerance. She was encouraged to increase resistance (and range for the shoulder abduction exercise) after demonstrating three or more consecutive days of either exercise without symptom aggravation the follow day (~24 hours post exercise completion).
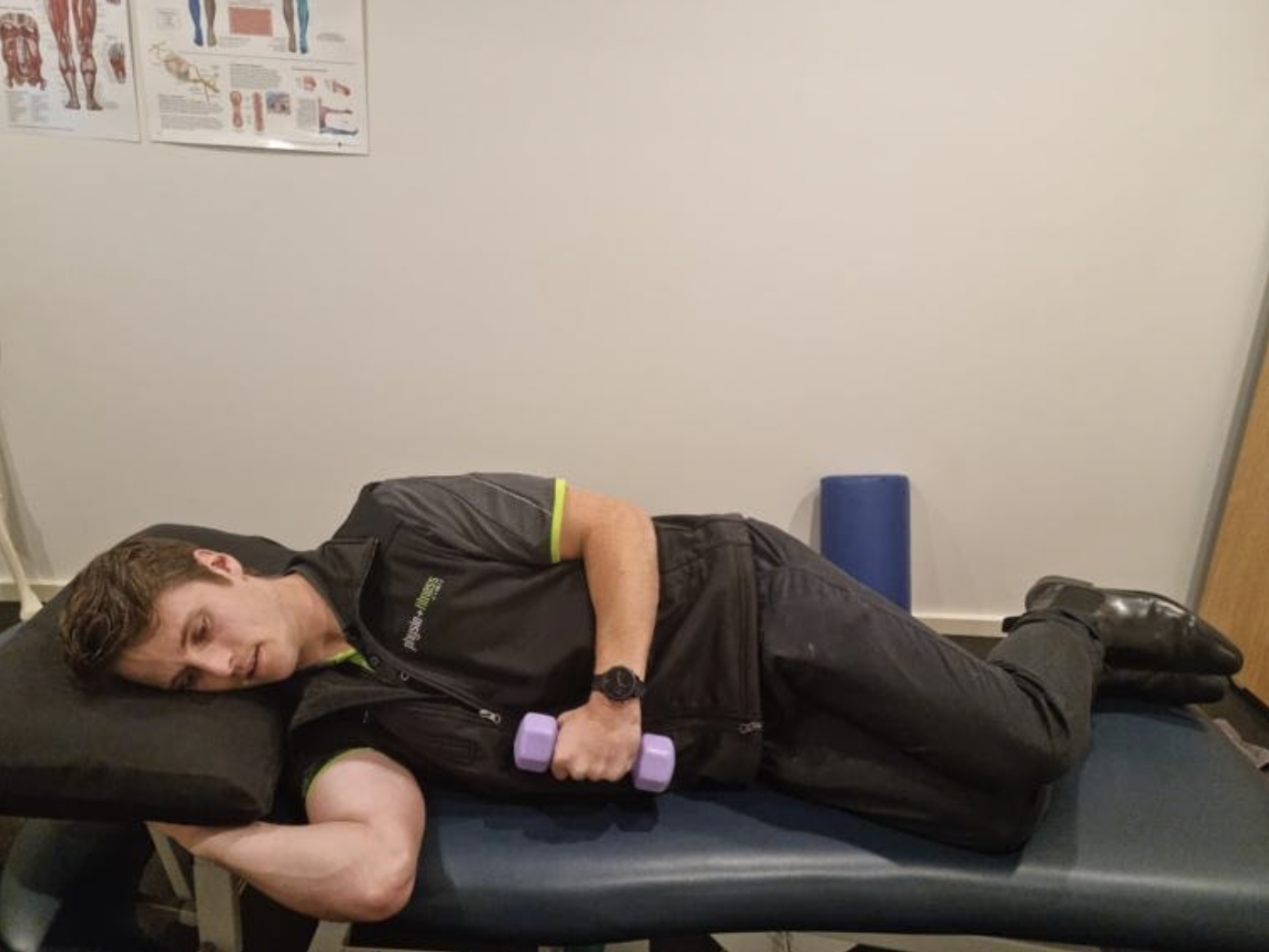
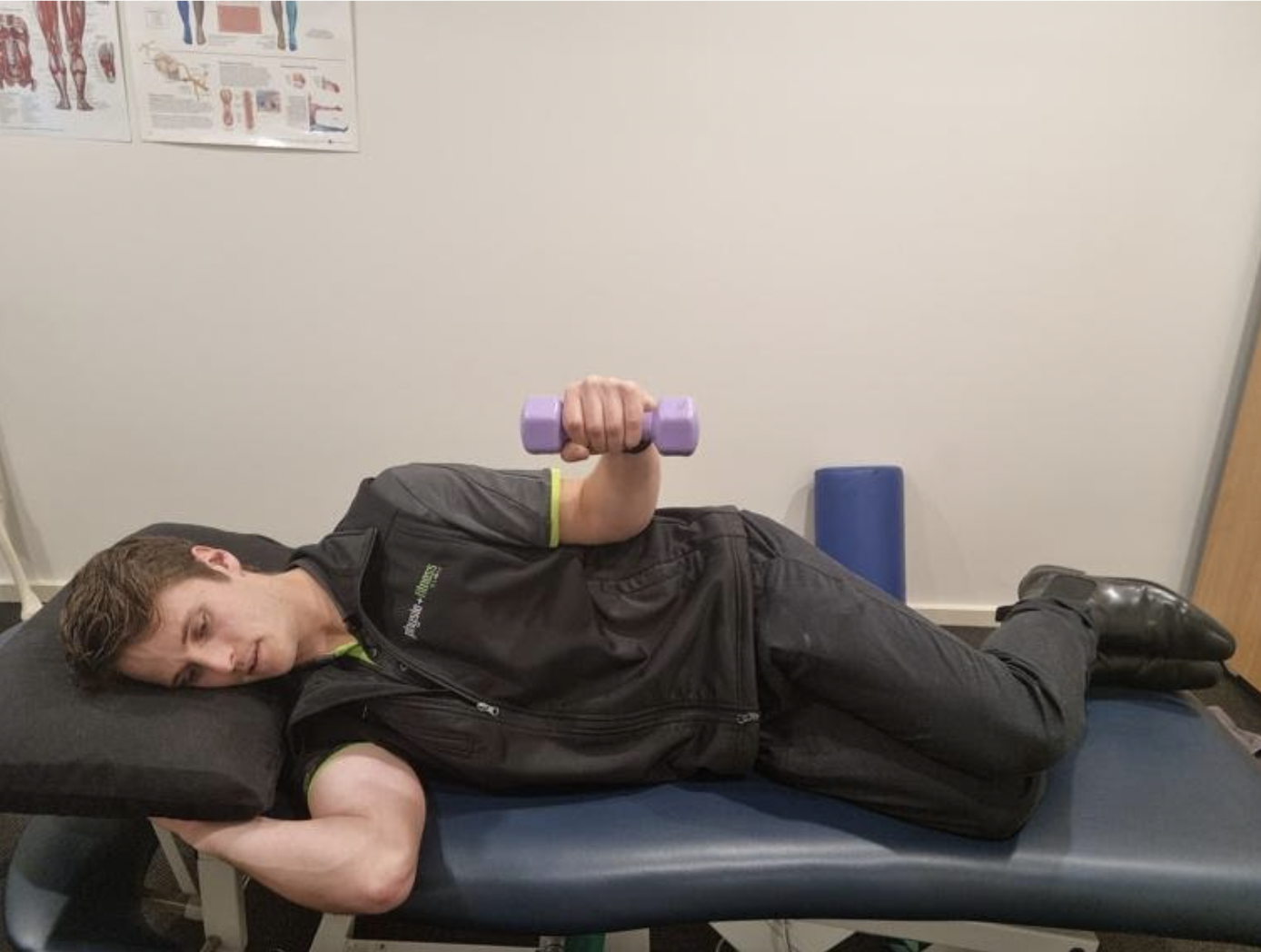
Figure one. Example of starting and end positions for side lying shoulder external rotation.
Pain management therapy was also provided to the client, in the form of soft tissue massage to all hamstring muscles (not the tendon insertion site). The client was shown foam rolling exercise, and instructed to use this for relief as required.
Within two weeks, the single leg isometric bridge was comfortable through range (isotonic), and was progressed accordingly. The client was educated on self-progression for the prone machine-based knee flexion exercise, whereby if this activity did not aggravate symptoms (per the pain threshold and delayed pain response established) after four repeats, and fatigue wasn’t being reached, an additional weight plate (2kg) was added.
After 6 weeks, Mrs S reported she experienced no pain with sitting or in the morning
Within three weeks of engaging physiotherapy, Mrs R demonstrated full pre-injury passive range of motion in all planes, and pain tolerable (but not pain-free) shoulder flexion active range of motion to 160 degrees. Per her physiotherapy plan, Mrs R had self-progressed the exercises prescribed, tolerating 3Kg side lying external rotation and 2Kg shoulder abduction to 90 degrees. Shoulder flexion resistance exercise was added at 2Kg as this was tolerated, and instructions matched to the shoulder abduction exercise (to increase range as is tolerated).
After 8 weeks of physiotherapy, Mrs R has achieved full active range of motion through all shoulder ranges, and only experiences mild shoulder pain with heavy overhead loading shoulder activity (>8Kg) or shoulder activity lasting for >1 hour. Importantly, she has also been able to garden without any restriction providing she takes regular breaks.
Discussion:
The diagnosis of rotator cuff related shoulder pain describes a clinical presentation of pain and impaired shoulder movement, particularly with overhead motion. This term is recommended in place of rotator cuff tendinopathy or shoulder impingement syndrome, and should encompass partial and full thickness rotator cuff tears, as there is no definitive way to determine if pain is resulting from the rotator cuff tendons or related tissue.
This diagnosis is made in the absence of serious pathology (e.g., resulting from trauma, cancer pain) or referred pain (i.e. cervical or thoracic radiculopathy). Additionally, for this diagnosis to be made, pain should not be resulting from a primarily stiff shoulder as would be expected with frozen shoulder, rather pain may be limiting range. Consider Mrs R, who had limited shoulder range actively but not passively.
Exercise is supported as the best intervention for rotator cuff related shoulder pain, with numerous studies reporting improved pain and reduced disability, with outcomes comparable if not better than surgery. Graded and progressive loading within pain tolerance limits, and that doesn’t result in prolonged symptom aggravation, is recommended. Mrs R, for example, experienced severe pain with most activity through active range. Initial exercise prescription focused on identifying tolerable exercise options that she could engage in. Following this, as pain improved, the exercise options were progressed (both in mode and in resistance applied) until meaningful functional capacity tolerances were met.
