Diagnosing Patellofemoral Pain Syndrome & Patella Tendinopathy
KNEE PAIN ASSESSMENT
FUNCTIONAL KNEE PAIN ASSESSMENT
The first step to assessing a patient that has come in with knee pain is a functional knee pain assessment. This involves a warm-up of 5 minutes then an examination using a variety of tests.
During these tests, the examiner will demonstrate how to perform the tasks and then observe their gait whilst standing and walking, how well they navigate stairs, and other movements such as knee extensions, making sure to compare both knees for any differences or weaknesses.
A Hop task is especially important for runners to assist with the diagnosis and treatment of their pain. are also assessed. The result of this assessment is then graded and used to come up with a treatment plan.
PATELLOFEMORAL PAIN SYNDROME
Patellofemoral pain syndrome encompasses discomfort in the front knee area, around the patella or kneecap. Often called ‘runners knee’ it affects athletes and is common in young people, more often females.
It occurs due to repetitive movements (usually from sports) or patella misalignment that cause the nerves within the knee to send pain signals from the muscles, tendons and cartilage to the brain. Patellofemoral pain syndrome can affect a person’s ability to climb stairs, kneel down or continue with daily activities because of pain and reduced range of motion.
Conservative treatment, like activity adjustments and therapeutic exercises, usually alleviates symptoms. Activities like running, jumping, and prolonged sitting worsen the knee pain. Rest, ice, and physical therapy are typical remedies.
PATELLA TENDINOPATHY
Patellar tendinopathy results from recurrent small tears in the patellar tendon that overtime heal and thicken to be a painful condition. It is frequently in young athletes involved in sports that involve vigorous jumping (basketball or volleyball). It presents itself as localized knee tenderness. The primary focus of treatment centers on conservative approaches, which involve decreasing activities that cause repeated stress on the knee. As pain diminishes, rehabilitation and functional recovery are accomplished through physical therapy and exercises. Surgery is typically reserved as a final option for persistent, unresponsive cases.
HOW PATELLOFEMORAL PAIN SYNDROME AND PATELLA TENDINOPATHY ARE DIFFERENT
Although both conditions present similarly and affect similar age groups, there is one main difference that helps distinguish the two. Patellofemoral pain often exhibits a broader and less precise distribution, ranging from beneath the knee to its outer, upper, or inner areas. Conversely, discomfort linked with the patellar tendon is specifically concentrated at the lower end of the patella. That’s one of the key things with tendinopathy is that it will stay on the tendon instead of moving around.
KNEE PAIN ASSESSMENT STEPS
These steps provide an example of the assessment process for a client with anterior knee pain:
- Have the client lie on their back for assessment.
- Observe the difference between the left and right thigh girth.
- Note any leg positioning variations, checking for natural leg rolling tendencies.
- Assess muscle tone variations, considering whether the leg falls forward differently on each side this would indicate muscle tone differences between the right leg and the left leg and that may be coming from higher up the kinetic chain (in through the hip and sometimes even the lower back).
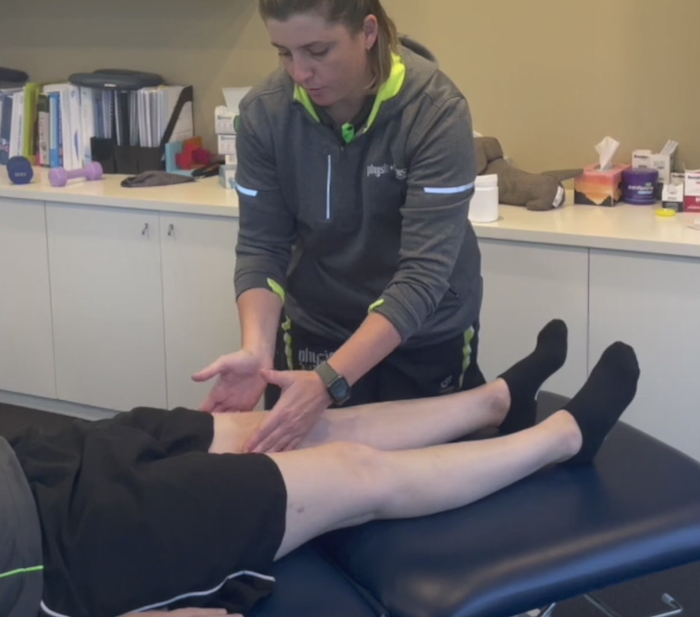
- Feel the knee and perform a “kneecap glide” to evaluate knee movement ease and client comfort level.
- Assess the “fat pad” at the front of the knee, a common pain source requiring distinct management.
- Evaluate the client’s range of movement and potential muscle imbalances.
- Compare quad activation by asking the client to press down their thigh, analyzing left-to-right differences.
Is patellofemoral pain syndrome the same as patellar tendinopathy?
No, they are two distinct conditions though both cause knee pain.
What is the difference between patellar tendonitis and patellar tendinopathy?
Whilst their symptoms are similar Patella Tendonitis and Patella Tendinopathy are actually different conditions. Patella tendonitis is inflammation to the tendon connecting the patella (kneecap) acute injury
Patellar tendinitis is an injury to the tendon connecting your kneecap (patella) to your shinbone. The patellar tendon works with the muscles at the front of your thigh to extend your knee so that you can kick, run and jump.
Patellar tendinitis, also known as jumper’s knee, is most common in athletes whose sports involve frequent jumping — such as basketball and volleyball. However, even people who don’t participate in jumping sports can get patellar tendinitis.
For most people, treatment of patellar tendinitis begins with physical therapy to stretch and strengthen the muscles around the knee.
Pain is the first symptom of patellar tendinitis, usually between your kneecap and where the tendon attaches to your shinbone (tibia)
Patellofemoral pain syndrome exercises
Stretches: calf wall stretch, quadricep stretch, hamstring stretch.
Exercises (to be 8-12 repetitions 2-3x per day):
Quadriceps strengthening:
- Sitting on the floor with one leg out straight in front and one bent up, placing a small towel under the knee of the straight leg. The client then presses the knee down into the towel by contracting the thigh muscle.
- Single leg raises: Laying down, one knee bent and the other leg straight on the ground. Slowly raise the straight leg using the thigh muscle until the foot is about 30 cm off the ground.
Hip Adductor Strengthening:
- Sit on a chair, place a softball in between your knees and try to squeeze your knees together and hold for 5-10 secs. Repeat as instructed above.
Does patellofemoral syndrome pain ever go away?
Up to 90 percent of those with patellofemoral pain syndrome achieve complete recovery from patellofemoral pain, enabling them to resume their usual activities. Although recurrence is possible, the likelihood diminishes with the implementation of prevention strategies.
How do I prevent knee injuries as an athlete?
Knee injuries can just happen though there are some strategies you can use. Always warm up before a workout and stretch afterwards to avoid injury.
Build strength, specifically in your legs and hips to improve knee stability.
Avoid deep squats as this can result in micro trauma to the tissues of the knee.
Don’t over do it, increase activity and weights slowly. Use appropriate footwear that is supportive and made for the activity you are involved in.
Consult a physio for safe movement techniques if you are concerned.
