Referred Pain from the Foot: An Overview of Symptoms, Causes & Treatments
Pain at the base of the foot can disrupt daily life and lead to discomfort that extends beyond just the foot itself.
It’s a condition that shouldn’t be ignored, as it can not only affect the foot but also cause referred pain in other areas of the body, such as the calf and knee.
In this article, we will explore the various causes and the importance of seeking assessment and treatment from a physiotherapist.
We’ll also discuss effective treatments and strategies for managing associated conditions to help you regain comfort and mobility.
Whether you’re an athlete dealing with overuse injuries or someone who experiences foot pain due to everyday activities, understanding the root causes and the impact on your overall well-being is essential. Gaining relief begins with a proper assessment by a physiotherapist who can identify the underlying issues contributing to your foot pain.
Muscles in the Arch of the foot
The arch of the foot is a remarkable structure supported by a complex network of muscles, tendons, and connective tissues. Here are some key components involved in maintaining the arch of the foot:
Plantar Fascia:
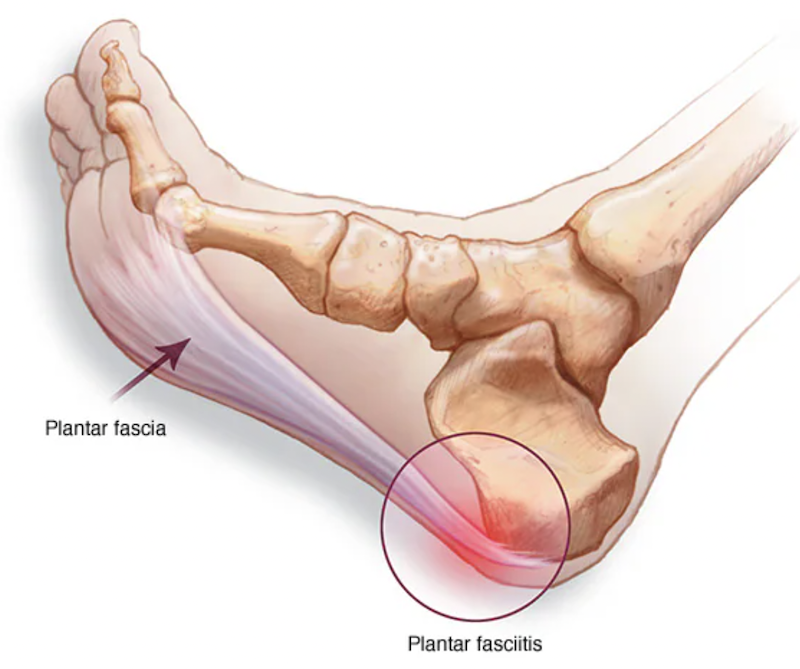
The plantar fascia is a thick and strong band of connective tissue that spans the underside of the foot, running from the heel bone (calcaneus) to the base of the toes.
Its primary role is to provide essential support to the arch of the foot, acting as a kind of natural “bowstring” that helps maintain the arch’s integrity. This crucial structure absorbs and distributes the weight and forces generated during walking, running, and other weight-bearing activities.
The plantar fascia also plays a role in connecting and holding together many of the small intrinsic muscles of the foot.
These intrinsic muscles are responsible for fine-tuning the movements and stability of the arch. They work in harmony to control the shape of the arch and adapt it to different activities and surfaces.
Flexor Hallucis Longus (FHL):
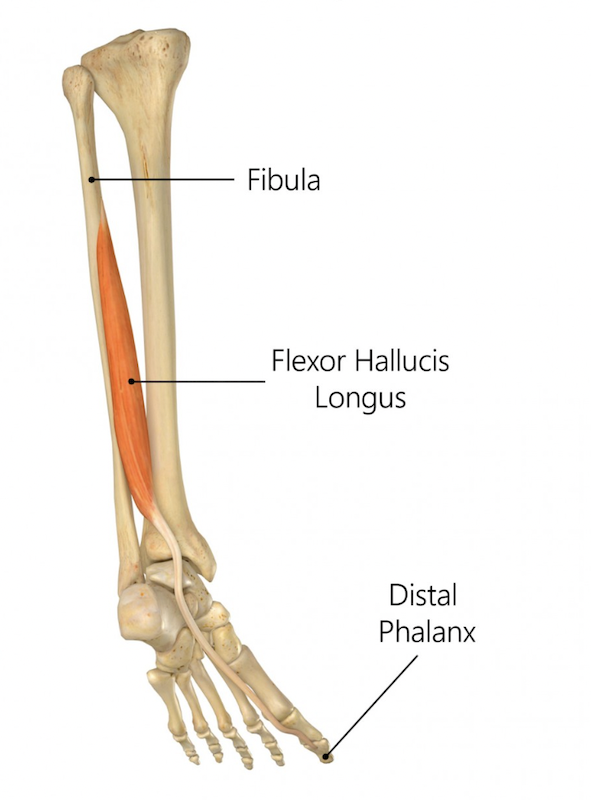
The flexor hallucis longus is a muscle located deep within the calf and foot. It plays a pivotal role in big toe movement.
When the FHL contracts, it flexes the big toe, allowing for actions like pushing off during walking and maintaining balance. This muscle is particularly important for activities that involve propelling the body forward, such as walking, running, and jumping.
The coordinated effort of these structures, including the plantar fascia, small foot muscles, and the flexor hallucis longus, helps maintain the arch of the foot’s stability and function.
Any disruptions or imbalances in this system can lead to conditions like plantar fasciitis or arch-related pain. Understanding the role of these components can be crucial for diagnosing and treating foot-related issues and ensuring that the arch of the foot functions optimally in various activities.
Flat foot, FHL & Associated Treatment

Flat feet, known as pes planus, can be attributed to various factors, including weaknesses and imbalances in foot muscles. Among these muscles, the flexor hallucis longus (FHL) plays a crucial role in supporting the arch of the foot. When the FHL is weak, the arch may collapse, resulting in a flat foot appearance. Conversely, tightness in the FHL can hinder the midfoot’s appropriate rolling during walking (gait), leading to biomechanical problems that affect not only the foot but also the calf and knee.
Physiotherapy offers effective solutions for flat feet associated with FHL issues. Treatment typically includes a combination of strengthening and releasing the FHL muscle to restore balance and function in the foot. A manual technique employed by physiotherapists involves using their thumb to run along the FHL muscle while mobilizing the big toe (dorsiflexion). This helps release muscle tightness and enhance flexibility, though it can be uncomfortable or painful, particularly when tightness is significant.
In addition to manual techniques, physiotherapists prescribe specific stretching exercises to increase FHL flexibility and strengthen it to better support the arch. Custom orthotic devices may also be recommended in some cases to provide arch support and correct gait abnormalities associated with flat feet.
What is Dorsiflexion?
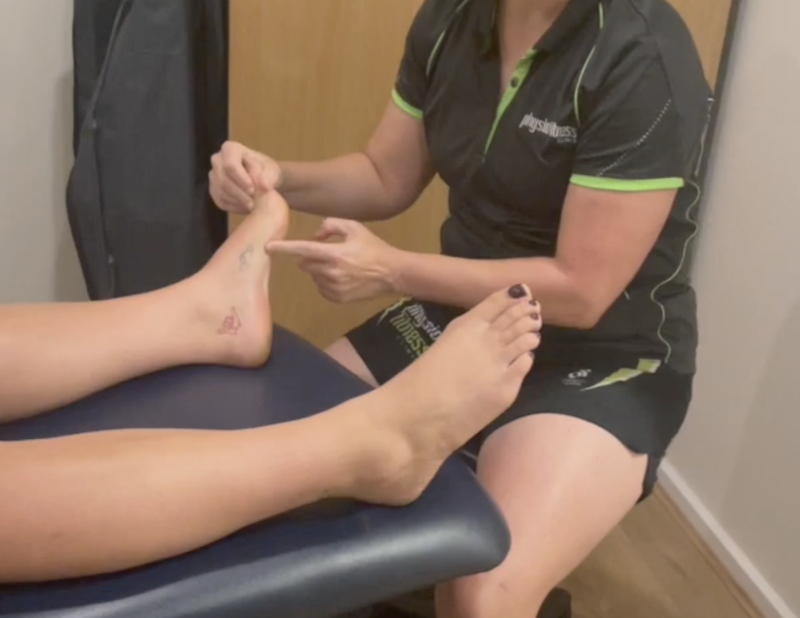
In the context of treating tight flexor hallucis longus (FHL) muscles, when a physiotherapist mobilizes the toe, this action is often referred to as dorsiflexion.
Dorsiflexion is a specific movement of the foot in which the toes are brought closer to the body. It is achieved by pointing the toes upward and towards the body as much as possible.
This motion helps stretch and release the FHL and can be a crucial component of therapy for conditions involving tightness in this muscle.
Conversely, the opposite movement is known as plantar flexion. Plantar flexion involves pointing the toes away from the body, typically achieved by pushing the toes downward and extending the foot.
What is the difference between flexible flat feet and rigid flat feet?

The key difference between flexible and rigid flat feet is in how the arch of the foot behaves.
Flexible flat feet have a normal-looking arch when not bearing weight (sitting or on tiptoes), but it collapses when standing.
Rigid flat feet have a flat arch that remains unchanged, regardless of the position of the foot.
Flat Foot Issues
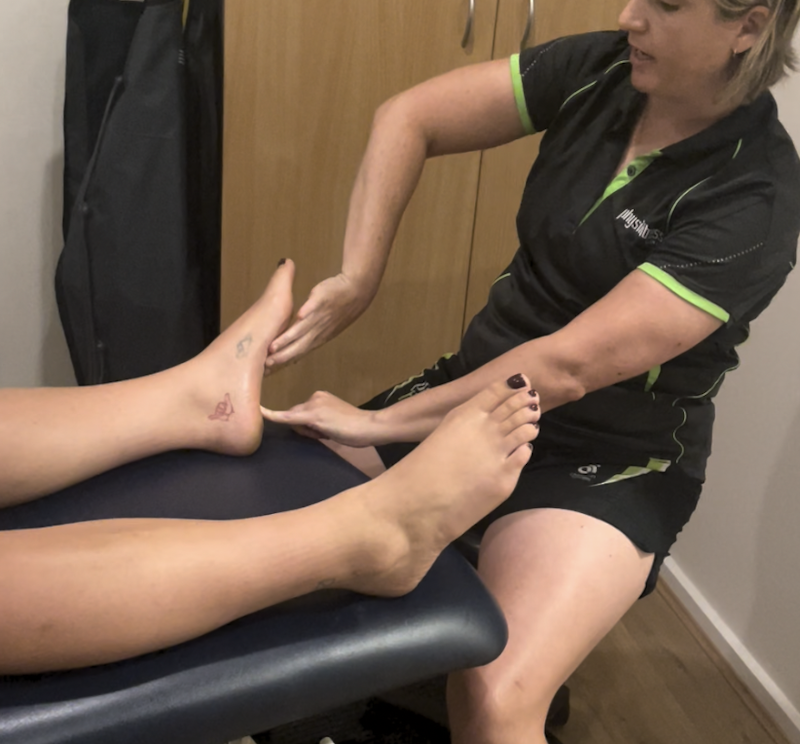
Flexible flat feet can lead to a range of symptoms and issues, including:
- Pain in Various Areas: Individuals with flexible flat feet may experience pain in the heel, arch, ankle, or the outside of the foot due to the altered foot mechanics.
- Ankle Pronation: Pronation is a natural inward rolling motion of the ankle when the foot hits the ground during walking or running. However, in flexible flat feet, this motion can become excessive, leading to overpronation, which can contribute to foot and leg pain.
- Shin Pain: The altered foot mechanics can also lead to pain along the shin bone (shin splints), as the muscles and tendons in the lower leg may be under increased stress.
Low Back and Knee Pain: The effects of flexible flat feet can extend beyond the feet and legs, potentially causing discomfort in the lower back and knees. This is often due to the altered alignment and biomechanics of the lower limbs.
Flat Foot Issues

Orthotic Devices: Orthotic insoles or shoe inserts are commonly prescribed to provide arch support and improve foot alignment. These devices can help alleviate pain and reduce overpronation.
Physiotherapy: Physiotherapists can use manipulation and massage techniques to address muscle imbalances and improve foot function. They may also recommend specific exercises to strengthen muscles that support the arch.
Activity Modification: Adjusting physical activities or sports to reduce the impact on the feet can be beneficial. Your physiotherapist can provide guidance on appropriate modifications.
Which deformity occurs due to flat foot?
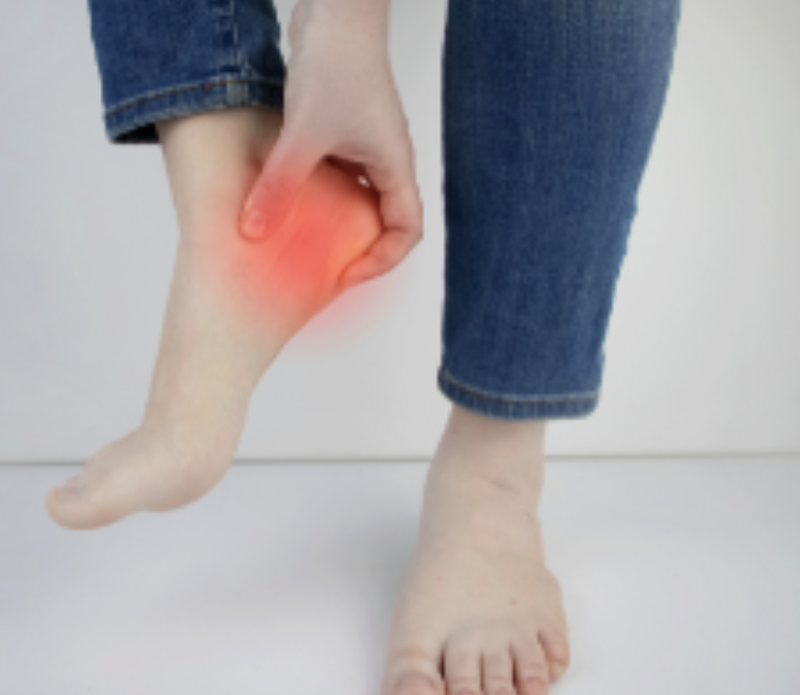
Posterior tibial tendon dysfunction
The deformity that occurs due to flat feet, particularly if left untreated, is posterior tibial tendon dysfunction (also known as posterior tibial tendonitis or adult acquired flatfoot deformity). Here are some key points about this condition:
Symptoms: Individuals with posterior tibial tendon dysfunction often experience pain on the inside (medial aspect) of the ankle and lower leg. The affected area will be sore to the touch. There may also be pain when performing a calf raise, along with noticeable weakness in the affected foot.
Aggravating Factors: Pain tends to worsen with weight-bearing activities like walking, running, or jumping. These activities place stress on the already compromised posterior tibial tendon.
Demographic Profile: This condition is more common in women around the ages of 40 to 50, though it can affect individuals of any age and gender.
Mechanism: Over time, repetitive stress and strain on the foot and ankle due to flat feet can lead to the weakening or degeneration of the posterior tibial tendon, contributing to the development of this deformity.
Treatment: Treatment options may include the use of orthotic devices (arch supports) to strengthen the arch and provide support to the affected foot. Lifestyle modifications, such as avoiding exacerbating activities, can also be helpful. In severe cases, surgical intervention may be necessary to correct the deformity and address the dysfunctional tendon.
