Piriformis Syndrome in Runners – Symptoms & Treatments
If you’re a runner and you’ve ever felt a sharp pain in the buttocks and sciatic nerve area, there are several diagnoses possible, including piriformis syndrome. We explain what it is and how we treat it.
The Piriformis Muscle
This condition occurs when the piriformis muscle, located in the buttock region, compresses the sciatic nerve. It can cause symptoms such as pain, numbness, and tingling, and can often be exacerbated by running, as well as other activities such as sitting due to the angle of the muscle.
Other Possible Sources of Pain
It is important to be properly assessed for Piriformis Syndrom and there might be a few other sources of pain in this region, including;
- Sciatica
- gluteal tightness
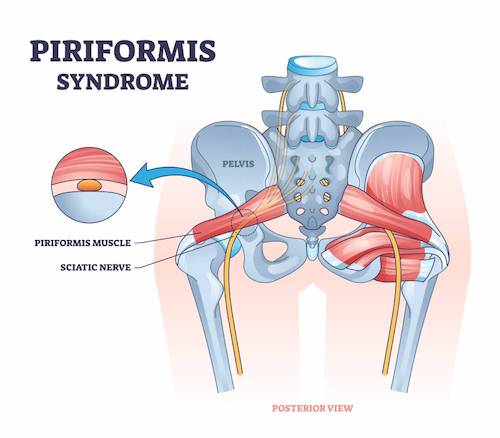
Piriformis Syndrome in Runners
There are several factors that can contribute to the development of piriformis syndrome in runners, including;
- Overuse
- Inadequate mobility of the hips
- Muscle imbalances
- Poor glute medius tone
- Tight hip flexors
- Tightness through the back – can contribute to the above mentioned issues, particularly in those who are driving large hours per week, and those in front of a computer all day.
Stretches to Prevent Piriformis Syndrome in Runners
To prevent Piriformis Syndrome, it is necessary to incorporate targeted stretching and strength training exercises into your routine, and gradually increase your mileage and intensity over time.
Obviously, this goes for all overuse based issues as well!
Every human is an individual, so it is important to find the right balance for yourself.
Stretches
Depending on your contributing factors, there are several exercises that can help with Piriformis syndrome.
HIP FLEXORS

Hip flexor stretch
SPIKEY BALL FOR GLUTES



Spikey balling your glutes is a simple yet effective exercise for runners dealing with piriformis syndrome
GLUTE BRIDGE
If the glute max is weak, glute bridges are a good, safe first exercise to commence with as it is low load and the movement pattern is unlikely to twist and load the piriformis excessively.

Glute Bridge
HIP FLEXOR STRETCH
CLAMSHELLS
If the glute medius is found to be weakened, clamshells are a good, simple exercise for the first phase of rehab, as it is light and again will not overload the piriformis.
WEIGHT BEARING + SINGLE LEG EXERCISES
Once these are activating well, then moving onto weight bearing and later single leg exercises are very important to creating a long term cure for the condition.
Piriformis Syndrome The FAQs
What is piriformis syndrome?
Piriformis syndrome is a condition characterised by pain caused by the irritation or compression of the sciatic nerve near the piriformis muscle.
The piriformis muscle plays an essential role in connecting the lowermost vertebrae to the upper part of the leg, passing through the “sciatic notch” in the pelvic bone.
This notch acts as a pathway for the sciatic nerve to travel into the leg. It’s important to note that because of their close proximity, problems can arise and cause discomfort.
Piriformis syndrome is a relatively common condition that affects the sciatic nerve, causing pain that radiates from the back or buttock into the leg, calf, and foot.
Research suggests that approximately 5% of sciatica cases can be attributed to piriformis syndrome. Interestingly, this condition appears to be more prevalent among women although the exact reason for this is still unknown.

What are 3 common causes of piriformis syndrome?
Piriformis syndrome can be caused by various factors that are recognized within the medical field.
These include;
- Injury
- Abnormal development
- Location of the piriformis muscle
- Sciatic nerve
- Abnormal spine alignment such as scoliosis
- Leg-length discrepancy where one leg is longer than the other
- Prolonged sitting especially with a thick wallet in a pocket behind the piriformis muscle
- Prior hip surgery
- Foot problems like Morton’s neuroma and unusually intense exercise routines.
However, it’s important to note that there are cases where the exact cause cannot be identified despite thorough evaluation and analysis.
Why do runners suffer from Piriformis syndrome?
Piriformis syndrome is a common issue that many runners face, and there are multiple factors that can contribute to its development.
Potential causes are;
- Overuse of the muscles,
- Limited mobility in the hips, and
- Muscle imbalances like weak glute mussels
- Tight hip flexors
Who else is prone to suffering from Piriformis syndrome?
Apart from runners, people who are often prone to suffering from Piriformis syndrome are;
- Individuals who spend long hours driving
- Those who spend long hours working at a computer may experience increased tightness in their back, which can further exacerbate these issues.
To avoid this condition, it’s important to include specific stretching and strength training exercises in your regular routine.
Additionally, gradually increasing your mileage and intensity over time can help prevent overuse-based issues.
It’s crucial to remember that every individual is unique, so finding the right balance for yourself is key.
What is the best way to get rid of piriformis syndrome?
There are various exercises that can be beneficial for treating Piriformis syndrome, depending on individual factors. One effective approach is foam rolling the glutes, ITB, hip flexors, and back.
Additionally, if weakness in the glutes is identified, starting with glute bridges can be a safe and low-load exercise to begin rehabilitation. This movement pattern minimises excessive stress on the piriformis muscle.
For individuals with weakened glute muscles, clamshells are recommended as an initial phase of rehab. This exercise is light and does not overload the piriformis. Once these exercises are successfully activating the targeted muscles, progressing to weight-bearing exercises and eventually single-leg movements becomes crucial for long-term recovery from Piriformis syndrome.
What aggravates the piriformis syndrome?
Preventing piriformis syndrome can be challenging as there is no foolproof method. However, for individuals who have experienced this or other back issues, there are some standard recommendations that may help alleviate symptoms and reduce the likelihood of future episodes.
These include;
- Practising home exercises and stretching routines,
- Considering a heel-lift if there is a discrepancy in leg length,
- Avoiding carrying a wallet in the back pocket,
- Minimising prolonged sitting periods
- Seeking treatment for any underlying contributing conditions such as spinal arthritis or foot problems.
If vigorous exercise triggers symptoms, it may be beneficial to decrease exercise intensity or switch to alternative activities like swimming instead of running to prevent recurrence in the future.
Does piriformis syndrome ever heal?
The duration of piriformis syndrome can vary. However, it is usually brief if proper treatment is initiated promptly after the onset of symptoms. By following the recommended treatment plan and proactive measures to support healing, individuals can successfully manage and overcome the challenges associated with piriformis syndrome.
What does an inflamed piriformis muscle feel like?
Those suffering from piriformis syndrome commonly experience symptoms that resemble sciatica, such as sharp and intense pain radiating from the lower back or buttock down to the leg, thigh, calf, and foot.
The piriformis muscle which is located in the buttock region puts pressure on the sciatic nerve which can lead to symptoms like;
- Pain
- Numbness
- Tingling
These symptoms may be mistaken for hip bursitis or a herniated disc, but a thorough examination can help identify the true cause. In addition to the aforementioned symptoms, individuals with piriformis syndrome may also face challenges when sitting or putting weight on one side of the buttock. They may have muscle spasms in the piriformis muscle and experience pain during a rectal exam. Furthermore, sciatica-like pain is often triggered when movement of the hip involves outward rotation against resistance.
What should I not do with piriformis syndrome?
There are several protective factors to consider implementing if suffering from piriformis syndrome;
- Avoiding carrying a wallet in your back pocket
- Limiting prolonged sitting
Seeking treatment for any other contributing conditions like spinal arthritis or foot problems may help. In addition, it’s important to be mindful of the activities you engage in. If vigorous exercise triggers your back pain, consider reducing the intensity or switching to low-impact activities such as swimming instead of running.
Should you stretch a sore piriformis muscle?
Piriformis syndrome can be managed and alleviated through various exercises, depending on the factors contributing to it.
One effective approach is foam rolling, which targets the glutes, ITB (iliotibial band), hip flexors, and back.
By incorporating these exercises into your routine, you can help relieve the symptoms associated with Piriformis syndrome.
What is the best position to sleep in with piriformis syndrome?
For optimal spinal alignment during sleep, it is recommended to either sleep on your back or, if you prefer sleeping on your side, place a pillow between your knees.
This will help keep your spine properly aligned throughout the night and promote better overall posture.
How do you tell if your sciatica is actually piriformis syndrome?
When experiencing potential conditions such as sciatica and gluteal tightness, it is crucial to undergo a thorough assessment by a medical professional. This will ensure an accurate diagnosis and appropriate treatment plan for any potential sources of discomfort or pain in this region.
How do I get my piriformis muscle to release?
There are various exercises that can help manage and alleviate the symptoms of Piriformis syndrome, depending on the factors contributing to it.
One highly effective approach is foam rolling, which specifically targets the glutes, ITB (iliotibial band), hip flexors, and back muscles.
By incorporating these exercises into your regular routine, you can significantly reduce the discomfort and symptoms associated with Piriformis syndrome.
How do you get rid of piriformis pain forever?
Although medications like pain relievers and muscle relaxants may be prescribed, the primary focus of treatment for piriformis syndrome lies in;
- Physical therapy
- Exercise
- Stretching
These non-invasive methods have proven to be effective in managing the symptoms associated with this condition. Some specific treatments that may be included in a comprehensive treatment plan are:
- Addressing gait adjustments to improve movement patterns.
- Enhancing mobility of sacroiliac joints through targeted exercises.
- Implementing stretches that specifically target tight piriformis muscles and other hip muscles.
- Strengthening the hip abductor muscles, which play a key role in outward hip movements.
- The application of heat therapy to alleviate pain and promote relaxation.
- Incorporating acupuncture as an adjunctive therapy option.
By focusing on these approaches instead of relying solely on medication, individuals with piriformis syndrome can achieve long-term relief and improved functionality. It is important to work closely with a qualified healthcare professional or physical therapist who can customize a treatment plan based on individual needs and goals.
If these initial measures do not provide sufficient relief, there are more advanced treatment options to consider, such as:
- Injections of a local anesthetic (similar to Novocain), botulinum toxin, or a corticosteroid agent. These injections are typically administered under the guidance of ultrasound, x-ray, or electromyogram to ensure accurate needle placement.
- Surgical intervention should be considered as a last resort. It involves removing a portion of the piriformis muscle or its tendon and has been reported to provide relief in cases that have not responded well to other treatments.
xxxxxxx
Prompt diagnosis and treatment are crucial for a positive prognosis.
Delayed diagnosis and treatment may lead to recurrent or chronic conditions with poorer outcomes.
Piriformis syndrome, although not widely known, can be a common cause of sciatic-type back pain. It is difficult to determine the exact prevalence as it may vary among individuals. However, if you experience persistent buttock pain that radiates into your leg and cannot find an explanation for it, there are some steps you can take.
Avoid carrying your wallet in your back pocket and try to reduce prolonged sitting. It’s important to consult with your health professional who can assess whether you have a disc problem or another common back issue, but they will also consider piriformis syndrome as a potential cause.
Interested in other Running Injuries? Check out our post on Running Injuries and Preventions.
